
What do you think of when you hear psychedelics? Let me guess: illegal and mysterious substances that can create a hallucinatory state of mind, commonly referred to as “getting high”? Your perceptions may change soon. Psychedelic substances are enjoying a rebirth of sorts in both the scientific community and popular media, vying to be a part of mainstream medicine. More and more scientific studies are being performed, producing positive results on the efficacy of psychedelics in treating different brain disorders. This scenario is common in the history of science. Psychedelic substances have long been used by the indigenous people of North and South America in traditional medicine and religion. The 1950s and 1960s also saw an upsurge of the use of these substances in the modern world for psychiatric treatment, but this progress was impeded by the counterculture movements of the 1960s in the West: an alternative cultural lifestyle born in response to various social and political issues like the Vietnam war, traditional authority, and women’s rights (Link). Psychedelics, an essential part of this movement, were used as a scapegoat, with government and media branding them dangerous and harmful. The culmination of these events led to the criminalization of these substances. Will the fate of psychedelics fate be any different this time around? Only time will tell. Nevertheless, it is high time to know more about these mysterious substances.
What are psychedelics?
Psychedelics are substances that can produce unique and distinctive changes in consciousness, the first-person experience by which we perceive the world inside and around us1. Some common examples of psychedelics are lysergic acid diethylamide (LSD) A.K.A. acid, psilocybin A.K.A. magic mushrooms, MDMA A.K.A. ecstasy, and dimethyltryptamine (DMT). There are important differences in the origins and actions of these different drugs. Some psychedelics can be found in nature (e.g., psilocybin, DMT) while others must be synthesized in laboratories (e.g., MDMA). At high doses, some psychedelics can also cause hallucinations (e.g., LSD, psilocybin).
How can psychedelics be useful in medicine?
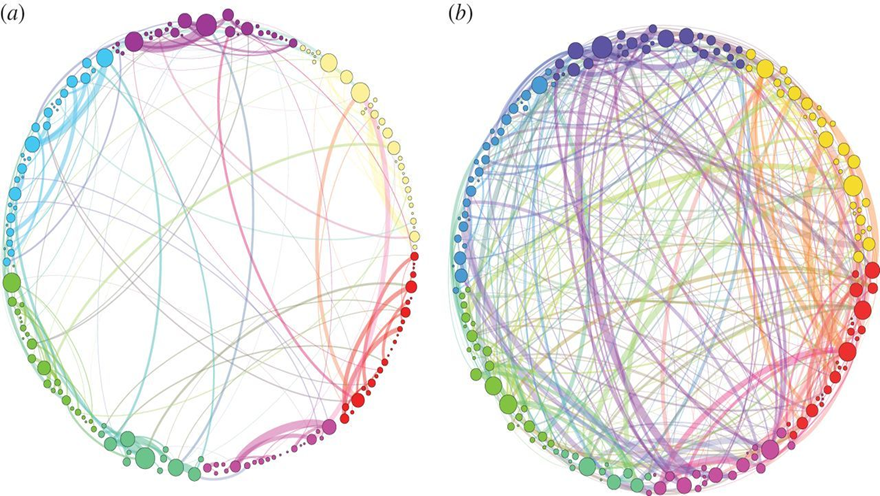
From a recreational or spiritual perspective, psychedelics have long been known to produce surreal or supernatural experiences, not commonly encountered in everyday life. But to be labeled as a medicine, substances must show beneficial effects in disease conditions. The key to how psychedelics might achieve this lies in the default mode network (DMN) of the brain. The DMN is composed of specific, interconnected regions of the brain which are activated when we are not focused on a particular task or problem. This state of daydreaming, when you are not focusing on the outside world, is known as the “resting state”. For a handful of us, we tend to think about what has gone wrong in our lives, why the future might be gloomy, or what others are thinking about us2. Thus, this network plays a vital role in depressive states like major depressive disorder that are characterized by such negative thought patterns. The DMN is also thought to be involved in other diseases and conditions like Alzheimer’s, autism, schizophrenia, and post-traumatic stress disorder (PTSD)2. Psychedelics can decrease the excessive activity and interconnections in the DMN3. On the other hand, psychedelics can also increase the structure and connectivity of neurons in other parts of the brain, which are not commonly active in the resting state. This decrease in hyperactivity in the ‘wrong areas’ and increase in connectivity in the ‘right areas’ can allow for a reboot of our resting brain network. In this way, psychedelics can have an incredibly positive effect on people’s perceptions, emotion, and thoughts about different situations, allowing patients with depression and addiction to find new meaning in life4.
What evidence is out there?
Drs. Robin Carhart-Harris and Guy Goodwin recently reviewed the therapeutic potential of psychedelic by examining existing research on the topic5. The current psychedelics ‘renaissance’ began with experiments in which psilocybin, a substance found in the magic mushroom, improved the emotional well-being of neurotypical volunteers. After that, LSD and psilocybin were used in terminal cancer patients who showed reduced symptoms of anxiety and depression over a sustained period. Psilocybin and ayahuasca also demonstrated beneficial effects in major depressive disorders. Psilocybin was particularly useful for depressed patients who did not respond to other therapies. Psilocybin has also shown benefits in treating addiction (smoking, alcoholism) and obsessive-compulsive disorder. Indeed, the FDA has designated MDMA and psilocybin ‘breakthrough therapies’ for PTSD as well as severe depression.
Potential pitfalls
It is important to keep in mind that medicinal uses of psychedelics were also heralded when these substances demonstrated therapeutic effects in mood disorders in research conducted between 1949 and 19736. However, inadequate research methodologies, unethical practices, and a spotlight on recreational drug-use nipped the science of psychedelics in the bud. Thankfully, current psychedelics researchers abide by rigorous scientific, ethical, and safety measures, which lends promise to the hope that history may not repeat itself. Yet, even if psychedelics emerge in mainstream medicine, we should not readily expect them to be available at a pharmacy or supermarket. Current clinical studies with psychedelics are being done under the supervision of health professionals (psychedelic-assisted psychotherapy) to achieve the maximum therapeutic benefit and manage possible side effects like psychosis. This supervised setting is vital for the safe and effective use of psychedelics in medicine.
What Now?
The potential impact of the use of psychedelics to treat mental disorders could be enormous. It could provide a much-needed thrust to break an impasse in the treatment of certain diseases such as chronic depression, the treatment of which currently involves long-term therapy, side effects, and resistance to traditional antidepressant drugs. The current boom in psychedelics research should be continued and expanded into larger population from different countries of the world under a controlled regulatory setting. This is important to the credibility and applicability of the research on psychedelics. History, as described above, must be carefully consulted to ensure a long-lasting future for psychedelics in mainstream medicine.
References
- Yaden, D.B., Johnson, M.W., Griffiths, R.R., Doss, M.K., Garcia-Romeu, A., Nayak, S., Gukasyan, N., Mathur, B.N., & Barrett, F.S. (2021). Psychedelics and Consciousness: Distinctions, Demarcations, and Opportunities. Int J Neuropsychopharmacol., 24(8):615-623.
- Buckner, R.L., Andrews-Hanna, J.R., & Schacter, D.L. (2008). The brain’s default network: anatomy, function, and relevance to disease. Ann N Y Acad Sci., 1124:1-38.
- Palhano-Fontes, F., Andrade, K.C., Tofoli, L.F., Santos, A.C., Crippa, J.A., Hallak, J.E., Ribeiro, S., & de Araujo, D.B. (2015). The psychedelic state induced by ayahuasca modulates the activity and connectivity of the default mode network. PLoS One., 10(2):e0118143.
- Swanson, L.R. (2018). Unifying Theories of Psychedelic Drug Effects. Front Pharmacol., 9:172.
- Carhart-Harris, R.L., & Goodwin, G.M. (2017). The Therapeutic Potential of Psychedelic Drugs: Past, Present, and Future. Neuropsychopharmacology., 42(11):2105-2113.
- Rucker, J.J., Jelen, L.A., Flynn, S, Frowde, K.D., & Young, A.H. (2016). Psychedelics in the treatment of unipolar mood disorders: a systematic review. J Psychopharmacol., 30(12):1220-1229.
Image References
- Pixabay.com Accessed 11/21/2021. Link
- Petri, G, Expert, P., Turkheimer, F., Carhart-Harris, R., Nutt, D., Hellyer, P.J., & Vaccarino, F. (2014). Homological scaffolds of brain functional networks. J R Soc Interface.,11(101):20140873.
